Where We Work
See our interactive map

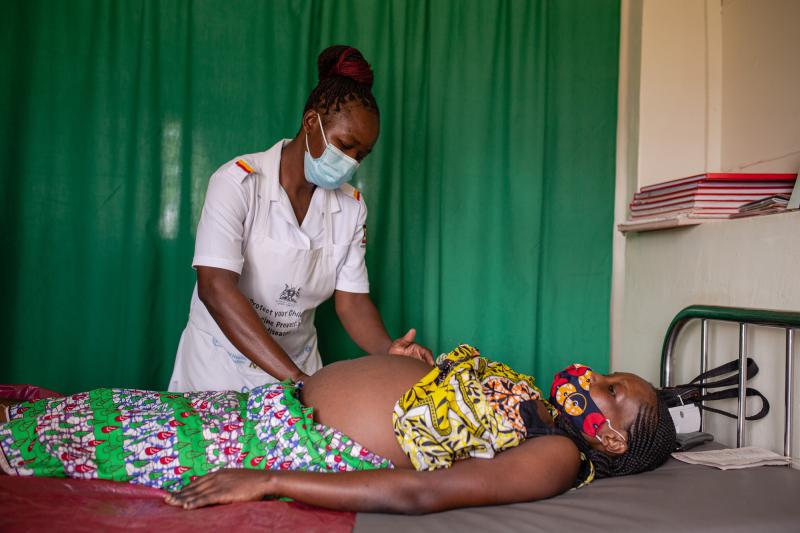
Nabukwasi Alice receives antenatal care at Nakaloke Health Center III in Mbale, Uganda. The USAID-funded RHITES-E Activity strengthened the capacity of health workers to provide high-quality integrated health services—including maternal and infant care, family planning, HIV, and more—in Eastern Uganda and Karamoja. Antenatal appointment attendance and facility births increased significantly. Photo by Esther Ruth Mbabaz for IntraHealth International.
As the first Africa Health Workforce Investment Forum kicks off, William Mubiru highlights what's worked in Uganda and what he hopes future investments focus on.
Next week the World Health Organization is holding the inaugural Africa Health Workforce Investment Forum, and will convene African ministers, donors, and civil society to stimulate and align long-term investment in the health workforce. These key decision-makers and actors will come to consensus around the first-ever Africa Health Workforce Investment Charter—which aims to cut the continent’s critical health worker shortage in half—and hammer out details to protect existing health workforce funding and partner on new investments.
I sat down with William Mubiru, a health systems and workforce expert in Uganda. Most recently he led the USAID-funded Regional Health Integration to Enhance Services in Eastern Uganda (RHITES-E) Activity and worked with the government of Uganda and partners to expand access to high-quality integrated health services in 30 districts in Eastern Uganda and Karamoja, home to over 7 million Ugandans.
Below he shares how his passion for improving the health workforce and access to health care is rooted in his childhood and home district, and what future investments should prioritize.
I was born and grew up in a community in Luweero District, which was at the center of the National Resistance Army war from 1980-86. The violence caused disruptions in service delivery, including health services, and breakdown of systems. Many health facilities were destroyed, and many health workers were killed or forced to flee. Lack of access to health care and essential medicines and inadequate numbers of health workers led to a high prevalence of diseases like malaria and diarrhea in my community.
We had to walk 15 kms each way to reach any health care services.
Even after the war we had to walk 15 kilometers, or about 3 hours each way, to reach any health care services. As I got older, I felt I needed to help the most vulnerable in my community, including the many widows and orphans, access health services. I ventured into public health to raise awareness about preventable diseases and work closely with the local leaders in lobbying for increased funding for the health sector.
The availability of health workers is still scarce, especially in rural and hard-to-reach areas. The country needs tens of thousands of additional skilled health workers to meet even the minimum targets required for UHC. We have weak leadership and governance for health workforce management. Many managers are not accountable and there's a lack of responsiveness to health workforce issues limiting access to care, like high levels of absenteeism. Another key challenge is poor data management. Because we still use multiple paper-based health information systems, especially at the community level, leaders don't have complete and aggregated data to make informed decisions.
The availability of health workers is still scarce, especially in rural areas.
Uganda struggles with limited domestic funds allocated to the health sector, and therefore for the health workforce. The current health budget is just 7.7% of the national pie, just half of the Abuja Declaration target. We also have poor community health systems, often characterized by inadequately trained and facilitated village health teams [VHTs]. The government is shifting to a more formalized community health workforce by piloting the Community Health Extension Workers Strategy, but this is yet to be adopted across the country.
There are lots of achievements, which I recommend should be replicated or sustained.
Localization. RHITES-E built the capacity of local partners, including three Regional Referral Hospitals, which are going to be critical in sustaining the gains we achieved. We worked with these partners to create capacity development plans and used several approaches like joint planning, mentorships, technical assistance, and “Data to Action” meetings. RHITES-E transitioned HIV/TB service delivery to these local partners and districts, and I'm proud that some of the districts—like Budaka, Kaabong, Manafwa, Mbale, and Sironko—were best performers in the Annual Health Sector Performance Report for 2022/23.
Health workforce development. RHITES-E worked with the Ministry of Health and regional referral hospitals to build the capacity of health workers in family planning; nutrition; maternal, neonatal, and child health; and emergencies. For example, during the upsurge of COVID-19, we worked with the national emergency department at the Ministry of Health to build the capacity of frontline health workers, especially midwives and nurses, in the areas of case management and home-based care, and to administer COVID-19 vaccinations, and this helped in reducing the fatalities of COVID-19.
Digital solutions. We built on existing technologies and platforms to improve data efficiency, from the community to the national level. For example, we supported the rollout of electronic medical records for antiretroviral therapy across 571 facilities in Eastern Uganda, and this led to improved timely district reporting into the national health management information system. We supported districts to roll out the national iHRIS human resources information system to collect information for workforce planning, deployment, recruitment, and attendance monitoring. District leaders used the iHRIS data for timely recruitment, and to fill more than 10,000 posts, while also reducing absenteeism.
Several districts used RBF funds to recruit health workers and increased facility births.
Result-based financing. The project supported the districts and the government of Uganda to roll out results-based financing [RBF], one of the key health financing strategies the country is embracing to improve service delivery. We worked closely with the ministry to build the capacity of districts to implement RBF and several districts, like Namisindwa, Kapchorwa, and Tororo, used RBF funds to recruit health workers, specifically additional midwives, which has helped improve service-level indicators, including increasing facility births.
Performance management needs to be prioritized—especially for improving health worker productivity, attendance to duty, and motivation—and also for holding health managers accountable for their own performance.
We need to invest more in the capacity of health workers. The country has invested in several strategies for health worker capacity development, but this needs to be amplified in all regions. We know this works—RHITES-E built health workers’ skills in integrated service delivery, and we saw huge increases in contraception use and in HIV viral load suppression for example.
We need to strengthen data management and invest more in digitalization of paper-based health information systems and building the capacity of all health leaders from community to the national level to use data for decision-making.
We need to improve public financial management and invest more in community health systems.
It’s critical to improve public financial management. As a country, a lot of our funding, especially for the health sector, is donor driven. Right now, over 40% of our national budget comes from donors. This calls for innovative approaches for enhancing efficiency in terms of resource allocation. There is need for investment in public financial management to minimize cases of corruption of public funds.
Finally, we need to invest more in community health systems and roll out paid, trained, equipped, and supervised community health extension workers to oversee VHTs and reach every single family, woman, and child and end preventable diseases and deaths. Most Ugandans live in rural communities that are far from health facilities. And this will help us a lot in minimizing the costs we are incurring for management of diseases.

Approximately 75% of Ugandans live in rural areas like Moroto, in Karamoja Region. Many people must travel long distances to reach a health facility. Photo by Tommy Trenchard for IntraHealth International. (Source: https://www.indexmundi.com)

William Mubiru [center] led the USAID-funded RHITES-E Activity, which expanded access to integrated health services in Eastern Uganda and Karamoja. Growing up during the NRA war, he remembers having to walk for hours to access any health care. Photo courtesy William Mubiru.

Mubiru says Uganda's critical shortage of health workers impedes equitable access today. The country needs tens of thousands of additional skilled health workers to reach minimum targets for UHC. Photo by Esther Ruth Mbabazi for IntraHealth International.

Additional health workforce challenges, like absenteeism, also impact access, especially for people in remote areas and the most vulnerable like children, people living with disability, and people living with HIV. Photo by Tommy Trenchard for IntraHealth International.

Uganda still has disparate paper-based health information systems, especially at the community level, making it hard for health leaders to make informed health workforce decisions. Photo by Tommy Trenchard for IntraHealth International.
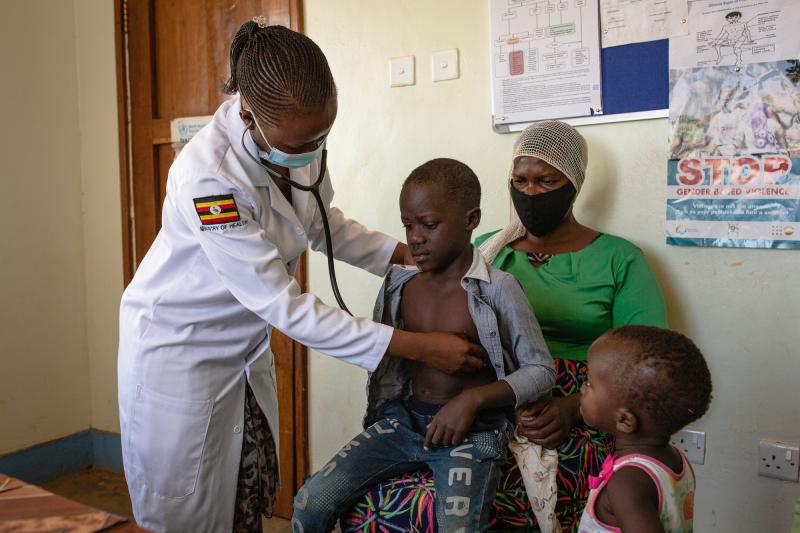
RHITES-E used health systems strengthening as its overarching approach to improving equitable access, building the capacity of local partners and fostering data-driven decision-making to strengthen local leadership. Photo by Esther Ruth Mbabazi for IntraHealth International.

High-quality integrated services improved through the project—including family planning; maternal, newborn, and child health; and HIV/AIDS—led to impressive results, such as increasing new users of family planning by 79%. Photo by Esther Ruth Mbabazi for IntraHealth International.

Smart investments in health workers work, says Mubiru. For example, RHITES-E provided over 70,000 HIV clients with antiretroviral treatment [ART] and achieved 93% viral load suppression among ART clients. Photo by Esther Ruth Mbabazi for IntraHealth International.

Mubiru has several recommendations for future health workforce investments, including focusing more on community health systems and paid and supported community health workers to reach every woman, child, and family. Photo by Tommy Trenchard for IntraHealth International.
Get the latest updates from the blog and eNews




